Screening diabetic neuropathy with SUDOSCAN in type 2 diabetes and prediabetes
Juan J. Cabré, Teresa Mur, Bernardo Costa, Francisco Barrio, Charo López-Moya, Ramon Sagarra, Montserrat García-Barco, Jesús Vizcaíno, Immaculada Bonaventura, Nicolau Ortiz, Gemma Flores-Mateo, Oriol Solà-Morales and the Catalan Diabetes Prevention Research Group.
Article title: Feasibility and Effectiveness of Electrochemical Dermal Conductance Measurement
for the Screening of Diabetic Neuropathy in Primary Care. Decoding Study (Dermal Electrochemical Conductance in Diabetic Neuropathy).
J. Clin. Med. 2019, 8(5), 598.
J. Cabré et al from Catalan Diabetes Prevention Research Group, Barcelona, Spain, analyzed the feasibility and effectiveness of dermal electrochemical conductance (DEC) measured with SUDOSCAN (quantitative expression of sudomotor reflex, generally called Electrochemical Skin Conductance, ESC) as a screening test of diabetic neuropathy (DPN) in primary health care centers.
Diabetic neuropathy (DNP) is the most common complication of diabetes and is of great clinical significance mainly due to the pain and the possibility of ulceration in the lower limbs. Early detection of neuropathy is essential in the medical management of this complication.
In patients with peripheral neuropathy, thin fibers (autonomic system—sweating) and thermal and tactile sensitivity are first affected, followed by the involvement of large fibers, presenting an altered vibrating sensation which eventually alters electromyography (EMG) patterns. Therefore, dysfunction of the sweat reflex in small distal fibers is one of the earliest changes detected in these patients.
This blind, prospective study included 197 people with type 2 diabetes (n=100), prediabetes (n=50) and normal tolerance (n=47), who underwent all the protocol tests and electromyography (EMG).
SUDOSCAN results (DEC, i.e., ESC) in the three groups are reported in the Table below:
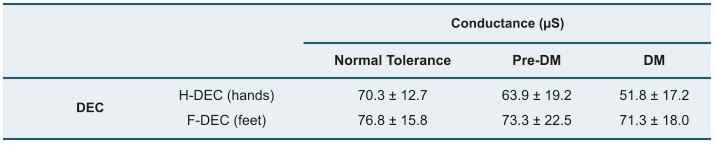
Comparison between DEC results in the three groups of participants
On comparing Dermal Electrochemical Conductance (DEC) with EMG as the gold standard, using area under the receiver operating characteristic (AUC, ROC curve analysis) the AUC was 0.65 in the diabetes population and 0.72 in prediabetes population. See ROC curve below.
Conclusion: in usual clinical practice, Dermal Electrochemical Conductance (i.e., ESC) in Diabetic Neuropathy is feasible, with moderate sensitivity but high specificity. It is also easy to use and interpret and requires little training, thereby making it a good screening test in populations with diabetes and prediabetes. It may also be useful in screening general populations at risk of neuropathy.
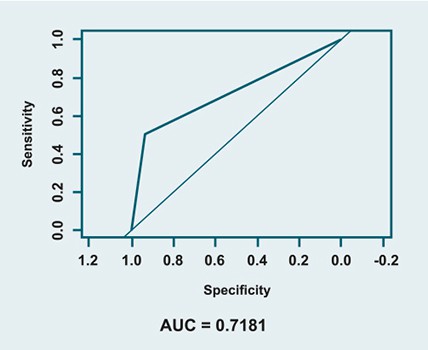
Receiver operating characteristic (ROC) curve of DEC versus electromyography (EMG) as the gold standard in the population with prediabetes.
Key words: dermal electrochemical conductance; diabetes mellitus; neuropathy; primary care; screening; sudomotor reflex.
Abstract available here.